Understanding Meningococcal Infection: A Comprehensive Guide to Transmission, Symptoms, and Types
Few infections evoke as much concern among parents and healthcare professionals as a Meningokokken Infektion. This bacterial illness can progress with alarming speed, potentially leading to life-threatening conditions like meningitis (inflammation of the brain and spinal cord lining) or sepsis (blood poisoning). The key to safeguarding against severe outcomes lies in rapid recognition and prompt medical intervention. But what exactly are Meningokokken, how do they spread, and what signs should you watch out for?
This article delves deep into the world of meningococcal disease, shedding light on its intricate mechanisms, vulnerable populations, and crucial preventative measures. Understanding these aspects is paramount for protecting yourself and your loved ones from this formidable pathogen.
What Are Meningokokken and How Do They Spread?
Meningokokken, scientifically known as Neisseria meningitidis, are bacteria that typically reside harmlessly in the nasopharynx – the upper part of the throat behind the nose – of a significant portion of the population. In fact, studies suggest that up to ten percent of people in countries like Germany can carry these bacteria without experiencing any symptoms themselves. These individuals are known as carriers, and while they remain healthy, they can inadvertently transmit the bacteria to others.
The transmission of Meningokokken primarily occurs through close, direct contact with respiratory secretions. This means activities involving the exchange of saliva or nasal fluids are common culprits. Think of kissing, sharing eating utensils or drinks, or being in very close proximity during sneezing or coughing. Dr. Franziska Roth, a senior physician at the Institute for Medical Microbiology and Hygiene, emphasizes that Meningokokken are quite delicate; they generally survive only for a short time outside the human body. This fragility means that casual contact or contact with contaminated surfaces is less likely to lead to an Meningokokken Infektion; direct person-to-person interaction is usually necessary.
So, if many people carry the bacteria without falling ill, what causes a severe infection? Dr. Roland Elling, a senior physician for Pediatric Infectiology, explains that in rare and not always fully understood circumstances, these bacteria manage to breach the protective mucous membrane barrier. Once this barrier is compromised, the Meningokokken can enter the bloodstream and, in some cases, even penetrate the central nervous system, leading to the devastating diseases associated with an invasive Meningokokken Infektion.
Recognizing the Dangers: Symptoms of a Meningokokken Infektion
The most concerning aspect of an Meningokokken Infektion is its potential to rapidly escalate into severe, life-threatening conditions. The two primary manifestations are bacterial meningitis and sepsis, each presenting with distinct but often overlapping symptoms. The challenge lies in the early stages, where symptoms can be non-specific and easily mistaken for common viral illnesses like the flu.
Symptoms of Meningitis (Brain and Spinal Cord Inflammation)
When Meningokokken infect the meninges (the membranes surrounding the brain and spinal cord), it leads to meningitis. Common symptoms include:
- Sudden high fever: Often the first sign, developing rapidly.
- Severe headache: Intense and persistent, often accompanied by sensitivity to light (photophobia).
- Stiff neck: Difficulty or inability to touch the chin to the chest. This is a classic, though not always present, sign.
- Confusion or altered mental state: Drowsiness, irritability, difficulty concentrating, or disorientation.
- Nausea and vomiting: Often accompanies the headache and fever.
- Seizures: Can occur as the infection progresses.
In infants and young children, symptoms can be more subtle and harder to identify. They might include irritability, lethargy, poor feeding, a bulging fontanelle (soft spot on the head), or a high-pitched cry. A stiff neck is often absent in very young babies.
Symptoms of Sepsis (Blood Poisoning)
If Meningokokken enter the bloodstream and multiply uncontrollably, it can lead to sepsis, a severe and widespread infection that can damage organs. Key symptoms of meningococcal sepsis include:
- Fever and chills: Often accompanied by shivering.
- Cold hands and feet: Despite a fever.
- Muscle aches and joint pain: Can be severe.
- Rapid breathing and heart rate: Signs of the body struggling to cope.
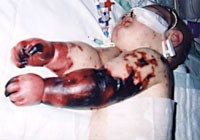
- Rash (petechiae or purpura): A distinctive feature of meningococcal sepsis. These are tiny red or purple spots that do not fade when pressed with a glass. This rash can quickly spread and indicates internal bleeding.
- Confusion and disorientation: As organs begin to fail.
Crucial Insight: The rapid progression of symptoms is a hallmark of meningococcal disease. What starts as a mild illness can turn critical within hours. If you suspect an Meningokokken Infektion based on these symptoms, especially the non-blanching rash, seek emergency medical attention immediately. Do not wait for all symptoms to appear. Early diagnosis and treatment with antibiotics are critical for survival and preventing long-term complications. For a deeper understanding of the urgency, read our article: Meningokokken: Why Rapid Detection is Crucial for Survival.
Who Is Most at Risk of a Meningokokken Infektion?
While anyone can contract a Meningokokken Infektion, certain demographic groups are significantly more vulnerable due to their developing immune systems or lifestyle factors that increase exposure:
- Infants and Young Children: Especially those under one year of age, have immature immune systems that are not yet fully equipped to fight off these bacteria.
- Teenagers and Young Adults: This group, particularly those living in close quarters such as dormitories, military barracks, or attending large social gatherings, is at increased risk due to frequent close contact and exchange of respiratory secretions.
- Individuals with Certain Immune Deficiencies: People with compromised immune systems, whether due to medical conditions (e.g., asplenia, complement deficiency) or certain medications, are less able to fend off the bacteria effectively.
The Many Faces of Meningokokken: Serogroups and Their Significance
Meningokokken are not a monolithic entity; they are classified into twelve distinct groups, known as serogroups, based on the composition of their outer capsule. These include A, B, C, E, H, I, K, L, W, X, Y, and Z. However, not all serogroups possess the same potential to cause serious invasive disease. According to microbiologists, the serogroups most commonly associated with invasive meningococcal disease (where the bacteria invade the body and cause illness) are A, B, C, W, X, and Y.
In Germany, data from the Robert Koch Institute (RKI) indicates that the vast majority of meningococcal infections are caused by just a few key serogroups: approximately 60 percent are attributable to serogroup B, about 20 percent to serogroup Y, and roughly 10 percent each to serogroups W and C. Other serogroups are comparatively rare in the region.
Understanding these serogroup distinctions is vital because vaccines are developed to target specific types. This allows for tailored protection against the most prevalent circulating strains.
Protection Against Meningokokken: Vaccination and Prevention
Vaccination stands as the most effective strategy for preventing a Meningokokken Infektion, particularly in the most vulnerable groups. The Standing Committee on Vaccination (STIKO) in Germany, for instance, issues clear recommendations for meningococcal vaccination:
- Meningococcal B Vaccination: STIKO recommends that infants receive vaccination against meningococcal serogroup B starting from two months of age. Catch-up vaccinations are advised up to the child's fifth birthday. The costs for this crucial vaccination are typically covered by statutory health insurance.
- Meningococcal ACWY Vaccination: While not universally recommended for all infants in Germany, vaccination against serogroups A, C, W, and Y is often advised for specific risk groups, such as teenagers before going to college, travelers to high-risk areas, or individuals with certain immune deficiencies.
It is generally advisable to complete vaccinations before children enter community settings like daycare or kindergarten, where the risk of transmission increases due to close contact. Beyond vaccination, general hygiene practices, such as not sharing drinks or eating utensils, can also help reduce the spread of respiratory droplets, though vaccination remains the strongest line of defense.
For detailed information on the vaccination schedule and who should be vaccinated, please refer to our dedicated article: Meningococcal Vaccination: Protecting Children At-Risk Groups.
Conclusion
A Meningokokken Infektion is a serious and potentially life-threatening illness that demands awareness and proactive measures. While these bacteria can reside harmlessly in the nasopharynx, their ability to rapidly invade the body and cause severe meningitis or sepsis makes them a formidable public health concern. Understanding the modes of transmission, recognizing the subtle yet rapidly progressing symptoms, and knowing who is most at risk are all vital steps in prevention and early intervention.
The development of targeted vaccines against the most prevalent serogroups, particularly B, C, W, and Y, offers robust protection. Following national vaccination recommendations, especially for infants and at-risk groups, is the most effective way to guard against this aggressive disease. In the face of suspected symptoms, particularly a non-blanching rash, immediate medical attention is not just recommended, but absolutely critical. Vigilance and timely action can significantly improve outcomes and save lives.